Discover how it works by scheduling a free consultation with our account specialist.
7 Pressing Truths about Modern-day Podiatric Practice Management
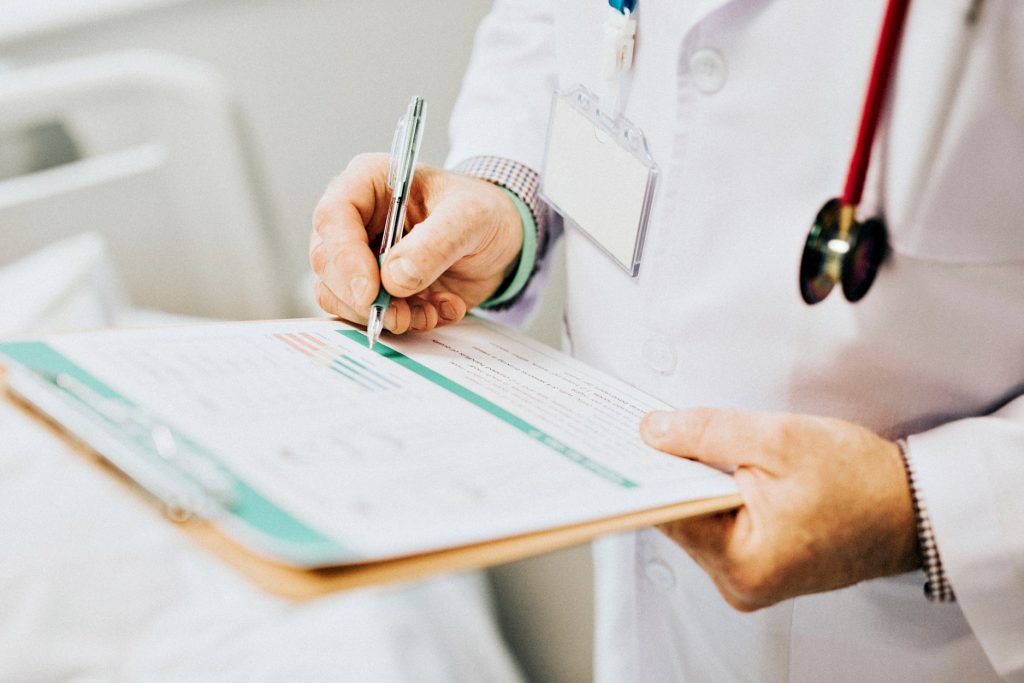
One-on-One with Pinnacle Practice Achievement’s Cindy Pezza
Early this year, Massachusetts Medical Society reported a crisis in health care across the United States. Physicians have reached critical levels of burnout, leading to poor administration of treatments and unhealthy lifestyles for physicians.
We sat with national practice management consultant Cindy Pezza to learn more about the current state of podiatric practices.

Cindy Pezza
Cindy is the President and CEO of Pinnacle Practice Achievement, a consulting firm dedicated to coaching podiatrists and their teams nationwide. Throughout her career, she has worked exclusively with podiatric professionals allowing her to incorporate her vast knowledge and experience in the field to establish and improve the health and sustainability of practices at every stage of the game.
Since 2002, she has immersed herself in the rapidly changing landscape of podiatric practices as well as the need to continuously evolve the methods by which they are managed. She has dedicated much of her life to traveling and educating podiatry students, residents, active providers and their staff members on the importance of establishing protocols and systems in order to achieve success.
Working with Pinnacle Practice Achievement (PPA), providers are able to utilize Cindy’s expertise to select the most effective program to help achieve their goals. From one-on-one custom consulting to convenient and cost-effective monthly subscription programs including access to a vast and expanding library of resources, monthly interactive webinars and exclusive vendor discounts, PPA offers what practices need the most to survive and thrive in the ever-changing world of specialty healthcare.
1. Physicians spend more time in paperwork
Physicians spend a large majority of their time trying to maintain compliance through the extensive documentation required for each patient encounter. According to Cindy, “It seems as though 75 percent of what they do now is paperwork and preparation. Diagnosing and treating is only a small piece of the puzzle.” This includes but is not limited to insurance verification of eligibility and benefits, electronic health record (EHR) charting, quality measure reporting and keeping up with changes in local and national coverage determinations.
Some physicians feel as if they are held hostage in the office hours after the last patient checks out just to complete their notes. She said, “Many are seeing a larger volume of patients to try and combat decreases in reimbursement so it seems nearly impossible to complete notes during the day. We are paperless but there’s more paperwork than ever.”
2. Developing systems is imperative and achievable
“Many doctors, when they are in residency have the mindset that it is too difficult to open their own practice so they must go and work for someone else,” she said. “But that is not necessarily the case. With the right vision, determination and a set of solid plans and goals, they can do it.”
Physicians often fear the challenges of starting their own practice and get lost in the process (sometimes before they begin). Part of Cindy’s role has been to prepare them mentally for the challenges that lie ahead. Tried and true protocols, systems and blueprints for establishing and building a sustainable practice guide them towards long-term success. It takes hard work and the ability to adapt to changes and setbacks as they arise, but if done properly, is well worth it.
3. Staff (the practice team) holds the key to practice success
Cindy often works with physicians and staff members collectively. Some meet as frequently (via video meeting or phone calls) as once a week while others keep in touch on a monthly basis to check in and make sure that established processes continue to move in the right direction.
PPA meetings include the entire team whenever possible (clerical, clinical and billing staff as well as physicians) so that all become more vested in the success of the practice. Topics of discussion vary widely and may include:
- the importance of customer service in the medical practice
- handling difficult situations/patients
- proper triage technique and scheduling
- updating of financial policies and collection processes
- further understanding treatment protocols and care plans
- incorporating additional or alternative ancillary products and services
- reputation management
The list continues to grow with the changing needs of practices but the basic concepts are the same.
According to her, “We are in the business of practicing medicine. Our patients are our customers and we need to do all that we can to keep them happy while maintaining control of the bottom line. Staff is the most important element of anything I do with the practice. If they are not on board with changes and improvements there is only so much that can be accomplished. The doctor is the captain of the ship but without the support of his/her crew, the ship has trouble staying afloat.”
4. Staff members need to be educated and trained
Running a successful practice includes lots of tasks that should be the responsibility of a well-trained staff. Without proper training and continued education, physicians often find themselves and their practices stuck in a plateau of sorts, unable to achieve their goals.
Cindy explained, “Doctors sometimes forget that staff members didn’t attend podiatry school or residency and very few (if any at all) have the ability to read minds. Staff members who understand why they are doing what they are doing and the benefit to patients and the practice are amongst the most valuable assets.”
5. Working harder for less pay
In an 8-hour clinic day, podiatrists treat an average of 30 patients varying by practice type, patient demographics and physician preference. Some podiatrists, however, are finding it necessary to see upwards of 50-70 patients per day because of decreases in reimbursement and increases in overhead costs.
Cindy commented, “The mentality is to fit as many patients as possible into the schedule in order to beat the system. What ends up happening is increased stress for doctors and staff (longer hours and more paperwork), a lack of following treatment protocols (skipping recommendations and discussions of treatment options in order to move patients in and out of the office as quickly as possible), delayed positive patient outcome (patients leaving the office without fully comprehending the care plan), longer wait times (leading to patient frustration and negative practice reputation), and a higher billing rejection rate (as insurance verifications fall to the wayside and simple human error rates increase). Long story short, they are spinning their wheels, making less for each visit and adding undue stress.”
6. Provider-patient relationship is at risk
Increasing compliance and documentation demands have made it extremely difficult for providers to build the kinds of positive and long-lasting relationships with patients that they did in the past. According to Cindy, many veteran physicians long for the time when they could spend the first ten minutes of a visit catching up on the kids and grandkids, treating the patient, jotting down a few sentences describing what was done and getting paid.
The practice was simpler, physicians could act as physicians and the care provided seemed more “meaningful” than in today’s world (how ironic). Over the past decade, doctors have been forced to shift their approach to practice management by reading Explanation of Benefits (EOB), studying Local Coverage Determination (LCD) guidelines and realizing that staying in the treatment room any longer than necessary may prove to be detrimental to their bottom line.
She urges her practices to manage their time in the treatment room wisely but also to consider the situation from a patient perspective imagining how it feels to explain how badly your heel hurts when you first step down out of bed in the morning while staring at a bald spot or at the backside of a doctor who is attempting to input all of the required information and complete a chart note by the end of your visit.
“Patients want to understand their condition and their treatment plan as thoroughly as possible without feeling like cattle being herded through the office. With increasing out of pocket expenses and non-covered services, patients are more serious than ever about the quality of care they receive and about getting better as quickly as possible,” she shared.
“If doctors are able to give their undivided attention during evaluation, treatment and presentation of the care plan, the patient leaves feeling as if they were heard and confident in the recommendations of the provider. The only way to accomplish this efficiently is to surround the physician with a team of support staff (in the office or remotely) who are well-educated, highly trained and all working together towards the success of the practice.”
7. Patient care and treatment are at risk
Cindy recalls incidences when staff would ask a patient prior to check out if they had any questions regarding their care plan (what they had to do at home following today’s visit, when they were to return, etc.) More often than not, the patient was confused and could not reiterate most of the information provided by the physician.
Patients would even confide in staff members that the doctor appeared rushed or distracted and they didn’t want to bother him/her by asking questions. It is important to remember that staff members are the eyes and ears of every practice as patients often relay information to a medical assistant or front desk receptionist that they never would to a doctor.
“Patients do not need very much of the doctor’s time but the time spent needs to have value,” she said. “Statistically, patients only require seven to eight minutes of face-to-face doctor time. They do however want to be listened to before the doctor begins reciting a rehearsed treatment plan and they want to feel that the support staff contributed to an overall experience that resulted in a high quality of care. A patient visit/encounter involves a lot more than time with the doctor in the treatment room, it is the entire experience from check in to check out that matters.”
Virtual Assistants in the Medical Practice
No matter how much healthcare changes or how drastically practice management has to evolve, PPA’s/Cindy’s fundamental goal remains the same; creating systems and protocols that allow providers and their teams to provide the highest quality patient care while maintaining a sense of controlled chaos throughout the clinical and clerical aspects of practice.
Working towards this goal often begins by helping physicians to improve their quality of life through delegation and the outsourcing of administrative tasks to virtual assistants.
Medical virtual assistants (MVAs) have proven to be great assets in the medical field and will continue to increase their value over time. They provide the much needed ancillary support that physicians need to make pivotal changes in their practices and in their personal lives.
“There will be a learning curve for a while when incorporating any type of virtual assistant, but initial efforts in the training and implementation process will yield significant results in the long run,” Cindy reported after speaking with Dr. David Laurino of Advanced Foot and Ankle Specialists of Arizona.
Dr. Laurino was elated to share his sense of accomplishment in leaving the office at 5:05 p.m. after treating his last scheduled patient at 4:45 p.m. just two weeks into working with a virtual scribe. Many other podiatrists report frequently working in the office hours past their last patient and then finishing notes at home until late in the evening.
External assistance allows physicians to regain a sense of balance between work and home, improving their quality of life and decreasing stress levels overall.
With solid systems in place, MVAs can work in a multitude of capacities from efficiently performing many of the behind the scenes tasks that office staff is unable to complete during busy clinic hours to working virtually along-side the doctor documenting each patient encounter. The tasks performed by MVAs produce smoother workflows while allowing more of the personal touches that are so often lacking in medical offices.
Mindset Shift for Improving Healthcare
“Doctors aren’t taught anything about running a business when they go to medical school,” Cindy explained. “They learn how to diagnose and treat patients and how to perform surgery. When it comes to managing a practice, doctors often don’t’ know what they don’t know and that can be dangerous.”
Physicians need to continually adapt the manner in which they manage their practices in order to stay up to date with trends. “If they are not constantly changing, improving and learning, they are falling behind.”
What situations and challenges have you observed in managing a podiatry practice? Let us know in the comments below! Don’t forget to share the love and tell your friends about the 7 Pressing Truths in Modern-day Podiatric Practice Management.
A special thanks to Cindy Pezza for gracing us with an interview. Information on private coaching and consulting packages, subscription programs and interactive monthly webinars are available through her website www.pinnaclepa.com. To hear from the expert in person, upcoming nationwide speaking events include the Civic Kern Hospital Alumni Association Annual Reunion May 1st-5th in Amelia Island, FL, the Ohio Foot and Ankle Medical Association Annual Meeting, May 17-19th in Columbus, OH Ohio Foot & Ankle Association and the Institute for Podiatric Excellence and Development Conglomeration, September 5-7th in Pittsburgh, PA IPED (September 2019).
Free consultations about hiring a virtual assistant for your practice are available through our inquiry page.
Stay Updated
Subscribe To Our Newsletter For Updates And A Free Copy Of The Bottleneck Medical Virtual Services Implementation Manual.

